Last updated on Apr 10, 2026

Stratis Health Wound Record Weekly Wound free printable template
pdfFiller is not affiliated with any government organization
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Stratis Health Wound Record Weekly Wound
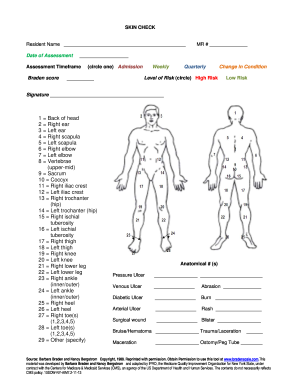
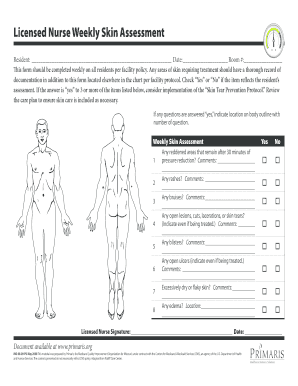
The Wound Record Weekly Wound Assessment is a healthcare form used by patients and nurses to document and track the status of a patient's wounds.
pdfFiller scores top ratings on review platforms




This is amazing. easy to use, intuitive. Have been looking for this type of product for years. Why did I not know about this before??
Takes a while to get used to changing documents. However, once you learn the rules it is easy to follow.
Who needs Stratis Health Wound Record Weekly Wound?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Stratis Health Wound Record Weekly Wound
What is the Wound Record Weekly Wound Assessment?
The Wound Record Weekly Wound Assessment is a critical healthcare form used for documenting and tracking the status of patient wounds. This assessment plays a vital role in ensuring that healthcare professionals maintain precise and accurate records of any wounds that a patient may have. Accurate wound tracking is essential for effective treatment and for monitoring the healing process.
Practitioners utilize this wound assessment form not only to record data but also to enhance communication among healthcare providers. This systematic approach to documenting patient wounds significantly contributes to improved patient outcomes.
Purpose and Benefits of the Wound Record Weekly Wound Assessment
The primary purpose of the Wound Record Weekly Wound Assessment is to provide a structured method for monitoring wound healing. This method benefits both healthcare providers and patients by ensuring that treatment is appropriate and effective. Systematic monitoring through this form enhances the quality of care offered to patients.
Some notable benefits include increased compliance with treatment protocols, better tracking of wound care progress, and timely adjustments based on patient needs. Overall, the assessment form serves as a valuable tool to bridge communication gaps between healthcare providers.
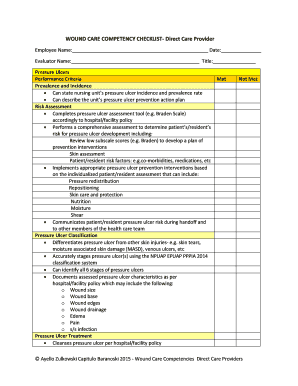
Key Features of the Wound Record Weekly Wound Assessment
This assessment form includes several key components critical for effective documentation. Essential sections include:
-
Patient information to identify individuals receiving care
-
Risk factors that may influence wound healing
-
Types of wounds documented
-
Treatment responses that indicate patient progress
Moreover, the form requires signatures from both the nurse and the patient, ensuring legal compliance and accountability in the documentation process.
Who Needs the Wound Record Weekly Wound Assessment?
The Wound Record Weekly Wound Assessment is particularly valuable for healthcare providers, including nurses and physicians, involved in wound care management. Eligibility for using the form is typically determined by the type and severity of the patient's wounds.
Patients with chronic, non-healing wounds or those requiring specialized care will often benefit the most from this assessment. By systematically documenting wound details, providers can better understand patient needs and tailor their approaches accordingly.
How to Fill Out the Wound Record Weekly Wound Assessment Online (Step-by-Step)
Filling out the Wound Record Weekly Wound Assessment online involves the following steps:
-
Access the form through the designated healthcare platform.
-
Complete the patient information section accurately.
-
Document any relevant risk factors affecting the patient’s wound.
-
Select the type of wound from the provided categories.
-
Detail the condition of the wound, including dimensions and treatment response.
-
Obtain signatures from both the patient and the nurse for validation.
Each section must include necessary details to ensure a comprehensive overview of the patient's wound status.
Common Errors and How to Avoid Them When Filling Out the Form
During the completion of the Wound Record Weekly Wound Assessment, users may encounter typical mistakes, such as:
-
Inaccurate measurements of wound dimensions
-
Omitting critical information in required fields
-
Lack of clarity in disclosures about the patient's condition
To avoid these errors, it’s essential to double-check all entries for accuracy and completeness. Ensuring that all required fields are thoroughly filled will enhance the form’s reliability.
How to Sign and Submit the Wound Record Weekly Wound Assessment
Signing and submitting the Wound Record Weekly Wound Assessment involves several processes. First, you can choose between a digital signature and a traditional wet signature. For digital submissions, it is crucial to consider security measures in place to protect sensitive information.
Available submission methods include electronic filing, which allows for immediate processing, and physical submission for those preferring hard copies. Understanding the advantages and limitations of each submission option can help ensure proper documentation handling.
Security and Compliance for the Wound Record Weekly Wound Assessment
Security is paramount when handling patient data. The Wound Record Weekly Wound Assessment complies with HIPAA and GDPR regulations, assuring that sensitive information is managed with the highest standards of protection. pdfFiller employs 256-bit encryption and adheres to SOC 2 Type II standards, ensuring robust data security.
These protocols help safeguard personal information while allowing healthcare providers to efficiently manage assessments without compromising confidentiality.
Sample of a Completed Wound Record Weekly Wound Assessment
Providing a visual or descriptive example of a completed Wound Record Weekly Wound Assessment clarifies how each section should be filled out. A properly filled-out form typically includes key components like patient details, wound types, and documented treatment responses, showcasing how thorough documentation supports effective patient care.
Each filled-out section is integral to understanding the overall status of the patient's wound, highlighting the importance of diligent record-keeping.
Experience Seamless Wound Assessment Management with pdfFiller
Engaging with pdfFiller for managing the Wound Record Weekly Wound Assessment can significantly streamline the form management process. The platform offers features such as editing, eSigning, and compliance assurance to make the completion of healthcare forms seamless.
By utilizing pdfFiller’s tools, healthcare providers can enhance their wound tracking process, ensuring effective monitoring and improving patient care outcomes.
How to fill out the Stratis Health Wound Record Weekly Wound
-
1.Access and open the Wound Record Weekly Wound Assessment form on pdfFiller by searching for it in the template search bar or browsing the healthcare forms category.
-
2.Once the form is open, familiarize yourself with the layout, including sections for patient information and wound assessment details.
-
3.Gather necessary patient information, including personal information, wound history, and treatment responses, to ensure all sections can be completed effectively.
-
4.Using the interactive fields, begin filling in the patient's personal information, ensuring accuracy with spelling and details.
-
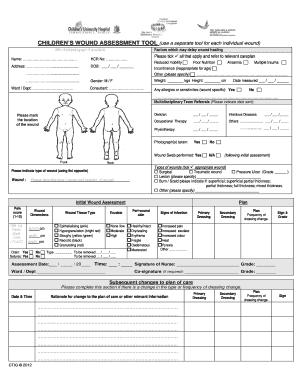
5.Navigate to the sections related to wound assessment, entering data on wound type, site, appearance, tissue quality, edges, drainage, and response to treatment.
-
6.Review each filled section for completeness, checking that no critical information is omitted and that all fields are accurately filled.
-
7.Once the form is completed, ensure the patient and nurse sign where required, using the signature fields provided on the form.
-
8.Finalize the form by reviewing all entered information, making any needed adjustments, and ensuring that it is ready for submission.
-
9.Save your work by clicking on the save option in pdfFiller, choosing your desired format such as PDF, or downloading it directly to your device.
-
10.If needed, submit the completed form via email or directly to the relevant healthcare provider using pdfFiller's submission features.

Who is required to sign the Wound Record Weekly Wound Assessment?
Both the patient and the nurse are required to sign the Wound Record Weekly Wound Assessment form to validate the information documented.
What should I do if I need assistance completing the form?
If you need help filling out the form, consider consulting with your healthcare provider or a nurse who can guide you through the necessary information and sections.
Are there any deadlines for submitting the Wound Record Weekly Wound Assessment?
There are generally no strict deadlines for submitting this form; however, it's best to complete and submit it promptly to ensure timely wound monitoring and care.
Can I fill out this form electronically?
Yes, you can complete the Wound Record Weekly Wound Assessment electronically using pdfFiller, which allows for easy input and saving of information.
What common mistakes should I avoid while completing this form?
When filling out the form, avoid leaving any required fields blank, ensure accuracy in all entries, and check that signatures are included where necessary.
Is notarization required for this form?
No, notarization is not required for the Wound Record Weekly Wound Assessment, simplifying the process for patients and nurses.
How can I access my completed form after submission?
Once you save or download the completed form through pdfFiller, you can access it from your device or account in pdfFiller for future reference.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.